Abstract
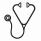
Background: Myeloproliferative neoplasms (MPNs) are a group of disorders of clonal hematopoiesis and include essential thrombocythemia (ET), polycythemia vera (PV) and primary myelofibrosis (PMF). Cardiovascular disease, including atrial fibrillation (AF), heart failure (HF), pulmonary hypertension (PH), and atherosclerotic heart disease, is an underappreciated cause of morbidity and mortality in MPNs. Additionally, MPNs harbor mutations commonly seen in clonal hematopoiesis of indeterminate potential (CHIP) which has been shown to be associated with increased cardiovascular risk. PH has been associated with MPN and MPN-associated PH is classified as group 5 PH according to the World Health Organization. Although studies have shown PH to occur in between 3.8% to 58% of patients with PMF and has been associated with decreased overall survival in PV, its impact on cardiovascular prognosis, including cardiovascular death (CV death), in patients with MPN has been understudied. Our study aims to investigate the prognostic implication of PH in a high risk MPN population, those with cardiovascular disease.
Methods: Our study is a single center retrospective cohort study. Using an institutional database, we identified 197 patients with MPN (ET, PV or PMF) who had cardiovascular disease (AF, hospitalization for HF or acute coronary syndrome after MPN diagnosis) and had undergone right heart catheterization (RHC) or transthoracic echocardiography (TTE). PH was defined as either a mean pulmonary artery pressure ≥ 20 mmHg on RHC or estimated right ventricular systolic pressure (RVSP) ≥ 50 mmHg on TTE. Our primary outcome was CV death (death due to pulmonary embolism, myocardial infarction, stroke, arrhythmia, sudden death or HF). Other outcomes of interest included all-cause mortality, HF hospitalization, VTE and arterial thrombosis. Continuous variables were compared using Student's t-test, categorical variables and outcomes were compared with the Fisher exact test. We used a Fine-Gray model to determine the effect of PH on CV death using other causes of death as competing events. To investigate the effect of PH on our outcomes we also used a multivariable logistic regression model using age, sex, MPN type, MPN treatment, arterial and venous thrombosis prior to and after MPN diagnosis, diabetes, prior HF diagnosis, HF hospitalization after MPN diagnosis, AF, hyperlipidemia, leukemic or secondary myelofibrosis transformation, and diabetes as co-variables.
Results: There were 92 patients with PH and 105 patients without PH. Median age at MPN diagnosis was higher in PH vs non-PH patients (73 vs 71, p = 0.038). The median time to diagnosis of PH from MPN diagnosis was 69 months (IQR 43, 113). Patients with PH had higher rates of prior HF (54% vs 32%, p = 0.001) and hypertension (83% vs 64%, p = 0.004), but lower rates of AF (64% vs 79%, p = 0.026) compared with patients without PH. MPN types and driver mutations were not statistically significant between PH and non-PH groups. More patients with PH had leukemic or secondary myelofibrosis transformation compared with patients without PH (23% vs 11%, p = 0.037). Patients with PH had higher rates of CV death (35% vs 9%, p < 0.0001), all-cause death (58% vs 37%, p = 0.004), HF hospitalization (73% vs 36%, p < 0.0001) and VTE (25% vs 12%, p = 0.027) but not arterial thrombosis (39% vs 41%, p = 0.88). Cumulative incidence of CV death was higher in PH compared with non-PH patients (Figure 1A, Fine-Gray HR 5.53, 95% CI 2.58-11.85). After multivariable regression, PH was associated with higher odds of CV death (Figure 1B, aOR 6.1, 95% CI 2.2-19.0), VTE (aOR 3.3, 95% CI 2.0-25.5), HF hospitalization (aOR 3.9, 95% CI 1.6-10.2) but not all-cause death (aOR 1.5, 95% CI 0.7-3.2) or arterial thrombosis (aOR 0.9, 95% CI 0.4-1.9), Figure 1B.
Conclusions: In patients with MPN and cardiovascular diseases, PH is associated with worse outcomes including CV death, VTE, HF hospitalization and leukemic/secondary myelofibrosis transformation compared with patients without PH. More investigation is needed but our results suggests early screening for PH may be beneficial in this patient population.
Neuberg: Madrigal Pharmaceuticals: Other: Stock ownership; Pharmacyclics: Research Funding. Rosovsky: Janssen: Consultancy, Research Funding; BMS: Consultancy, Research Funding; Inari: Consultancy, Membership on an entity's Board of Directors or advisory committees; Dova: Consultancy, Membership on an entity's Board of Directors or advisory committees. Hobbs: Bayer: Research Funding; Incyte Corporation: Research Funding; Merck: Research Funding; Constellation Pharmaceuticals: Consultancy, Research Funding; Novartis: Consultancy; Celgene/Bristol Myers Squibb: Consultancy; AbbVie.: Consultancy.
Author notes
 This icon denotes a clinically relevant abstract
This icon denotes a clinically relevant abstract

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal